
Microbiome oncology represents a paradigm shift in pancreatic ductal adenocarcinoma treatment
• Introduction: The Silent Killer and the Second Genome
Oncology is hitting a pivot point. For decades, pancreatic ductal adenocarcinoma (PDAC) has been the "silent killer," defined by a brutal statistical reality: in 2020 alone, the world saw 495,773 new diagnoses and 466,003 deaths.
When mortality nearly mirrors incidence, the message is clear: our current strategies are failing. With a five-year survival rate stuck between 10% and 13%, the medical community has long viewed the pancreatic tumor as an impenetrable fortress.
But we've been looking at the wrong blueprint. A fundamental shift toward a meta-organismal perspective is revealing that the human body is not a closed system, but a complex ecosystem. By interrogating the "second genome"—the human microbiome—scientists are finding that these microbial hitchhikers are pivotal regulators of how cancer grows, evades the immune system, and resists treatment.
The Magnitude of the Problem
Pancreatic cancer is the fourth leading cause of cancer death in developed countries. When diagnosed, 80-92% of cases are already inoperable. Median survival for metastatic disease is only 6-9 months.
1 Your Saliva as a Crystal Ball: The Oral-Pancreas Axis
The journey to the pancreas begins in the mouth. We now know that the mouth and pancreas are linked via a biological highway; periodontal pathogens translocate through the bloodstream or swallowed saliva, setting up shop in the pancreas to trigger chronic inflammation and "parainflammation."
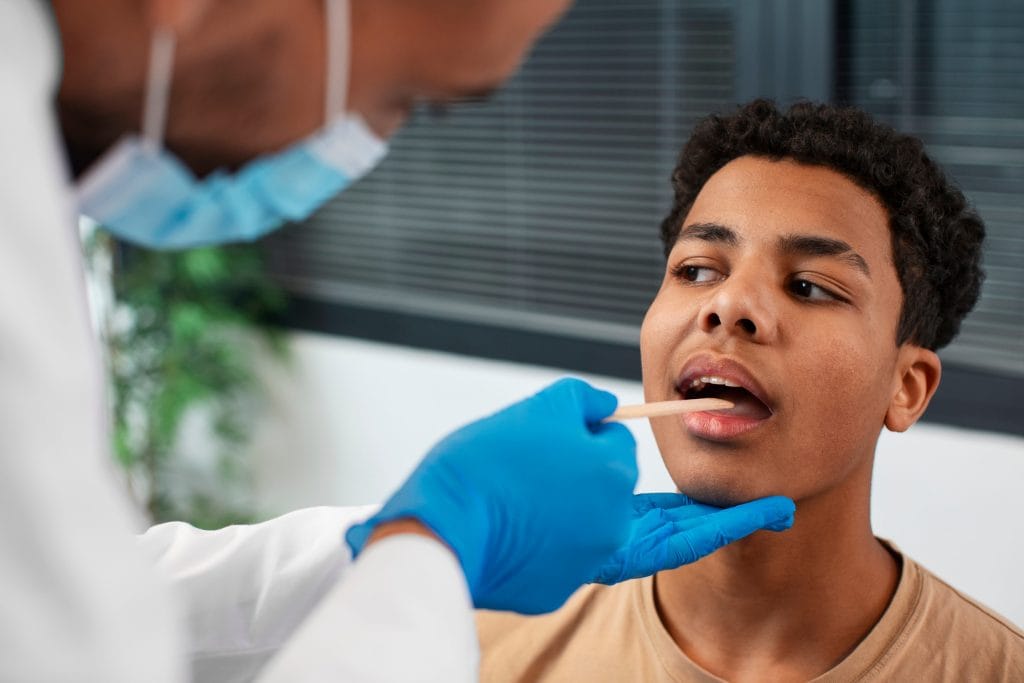
Non-invasive salivary testing could revolutionize early pancreatic cancer detection
This "Oral-Pancreas Axis" has yielded a breakthrough in early detection: the Microbial Risk Score (MRS). By analyzing 27 specific oral species—including Porphyromonas gingivalis and Eubacterium nodatum—researchers can identify individuals with a 3.5x greater risk of developing PDAC.
The Mycobiome: The Molecular Villain
The mycobiome (fungal community) adds another layer of complexity. While Candida tropicalis is linked to higher risk, the Malassezia genus is the true "molecular villain," driving oncogenesis by activating the mannose-binding lectin (MBL) pathway and triggering the secretion of IL-33, which creates an immunosuppressive "shield" around the tumor.
"A collection of 27 specific oral microbial species [are] tied to a 3.5 times greater risk of developing PDAC... pathogens can translocate from the oral cavity to the pancreas via the bloodstream or swallowed saliva, inducing chronic inflammation and oncogenic signaling." — Meng et al., JAMA Oncology 2025
Why It Matters
A non-invasive "salivary diagnostic" tool would be a total game-changer. Given that only 8–20% of cases are caught while still resectable, a simple mouthwash test to calculate an MRS could provide the early warning system we have lacked for half a century.
2 The "Survival Blueprint": Why Some Patients Beat the Odds
The old dogma claimed the pancreas was a sterile organ. We now know the opposite: the cancerous pancreas is a thriving, diverse ecosystem. Interestingly, the composition of that ecosystem determines who lives.

The gut microbiome: a complex ecosystem influencing cancer response
In a landmark study published in Cell, researchers decoded the "Survival Blueprint" of Long-Term Survivors (LTS)—those rare patients surviving more than five years. These survivors harbor a specific signature of four bacterial taxa:
- Pseudoxanthomonas
- Streptomyces
- Saccharopolyspora
- Bacillus clausii
This microbial quartet is an active defense system, not just a marker. It predicts long-term survivorship with a staggering Area Under the Curve (AUC) of 97% to 99%. These microbes act as cellular recruiters, calling in CD8+ cytotoxic T cells to the tumor microenvironment to hunt and destroy cancer cells.
3 The Chemotherapy Hijack: Why Bacteria "Eat" Your Meds
One of the most frustrating hurdles in PDAC treatment is drug resistance. A paradigm-shifting discovery has revealed a bizarre cause: the bacteria are literally metabolizing the medicine.
Intratumoral Gammaproteobacteria express an enzyme called cytidine deaminase, specifically the long isoform (CDDL). This enzyme "eats" Gemcitabine—the standard-of-care chemotherapy—converting it into an inactive, useless form.
The Pivot: A Simple Solution
There is a dark irony in a life-saving drug being neutralized by a microbial passenger. However, the solution may be remarkably simple. Preclinical data suggests that common antibiotics like ciprofloxacin can clear these bacteria, reversing resistance and potentially extending survival in metastatic patients by several months.
"Intratumoral bacteria express cytidine deaminase that metabolizes gemcitabine, converting the first-line drug into an inactive form. Antibiotics can reverse this bacterial resistance." — Geller et al., Science 2017
4 Re-Engineering the Gut: Fecal Transplants and Immunotherapy
If certain microbes help patients survive, can we "program" that resistance into others? The evidence points to a resounding yes. Fecal Microbiota Transplantation (FMT) is moving from the lab to the clinic as a way to "reset" the gut-immune axis.
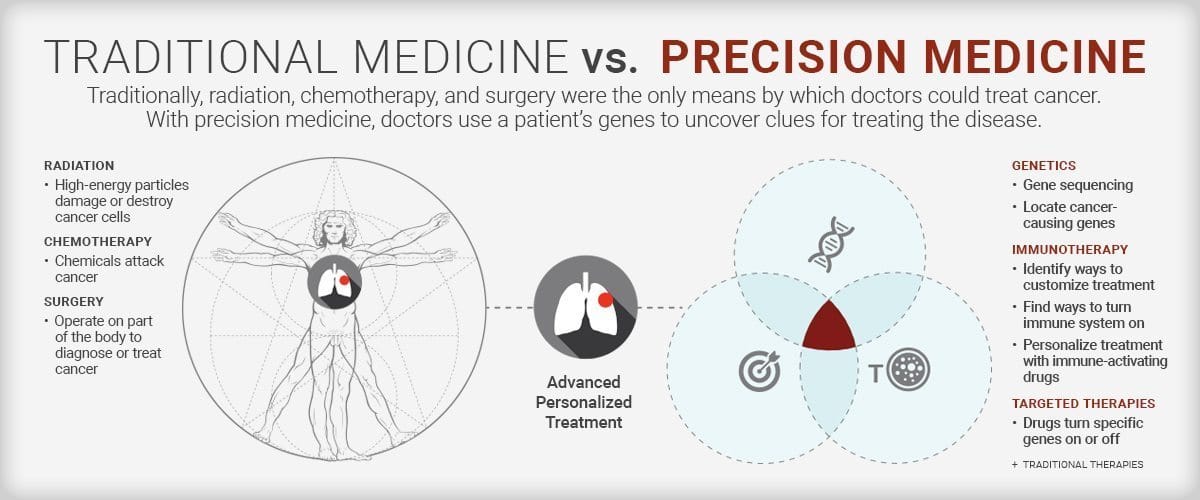
Microbiome-based precision medicine represents the future of oncology
In mouse models, FMT from long-term survivors reduced tumor growth by 70%. The human results are even more provocative. A 2026 case report documented a patient with refractory advanced cancer who received FMT combined with pembrolizumab and γδ T cell therapy. The result? Significant tumor shrinkage and the normalization of the CA19-9 biomarker to 72 U/mL.
Clinical Results
FMT from LTS donors into mouse models has been shown to reduce tumor growth by 70% compared to STS (Short-Term Survivor) transplants. Human trials are showing similarly promising results.
5 Breaking the "Armor" with Hyperbaric Oxygen
The physical architecture of a pancreatic tumor is its greatest defense. It is wrapped in a "dense, desmoplastic stroma"—a suit of biological armor made of collagen and fibronectin that chokes off blood flow and blocks drugs.
To crack this armor, researchers are using Hyperbaric Oxygen Therapy (HBOT) to shift the tumor from a state of "suffocation" (hypoxia) to "normoxia." By raising tissue oxygen from a measly 5 mmHg to a robust 30–50 mmHg, HBOT triggers reactive oxygen species that physically degrade the matrix.
Mechanism of Action
This "oxidative degradation" reduces collagen by 35% and fibronectin by 30%, thinning the armor so nanodrugs and immune cells can finally penetrate the target.
6 The Molecular Twin: AI Meets the Microbiome
The future of pancreatic oncology is a synthesis of biology and big data. We are no longer guessing at outcomes; we are simulating them.
- The Molecular Twin: This AI platform integrates clinical data with 6,363 multi-omic features, including microbial signatures, to predict survival with 87% accuracy.
- PDACensus: By using machine learning to map the relationship between the tumor and its surrounding stroma, this algorithm achieves diagnostic accuracies exceeding 96%.
This represents the ultimate precision: using thousands of data points to build a digital replica of a patient's disease, allowing for personalized "microbiome-guided" therapy before the first dose is ever administered.
• Conclusion: Toward a Programmable Axis
The microbiome is no longer a peripheral concern; it is a programmable axis that offers us the first real chance to influence the "unbeatable" nature of pancreatic cancer.
From the salivary signatures that flag risk to the microbial enzymes that hijack chemotherapy, the "second genome" is the key to the next generation of oncology. We are entering a meta-organismal future where cancer management is as much about ecology as it is about genetics.
The Future of Detection
The next time you face a cancer screening, it may not involve a biopsy or a radiation-heavy scan. It might just start with a simple mouthwash or a gut-health check. Are you ready for the era of programmable medicine?
Key Takeaways
- Oral microbiome can predict PDAC risk with 3.5x greater accuracy
- Four bacterial taxa predict long-term survival with 97-99% accuracy
- Intratumoral bacteria metabolize gemcitabine, but antibiotics can reverse this
- Fecal transplant from survivors reduces tumor growth by 70%
- AI with microbial signatures predicts survival with 87% accuracy
Scientific References
"Tumor Microbiome Diversity and Composition Influence Pancreatic Cancer Outcomes"
Cell, 2019
DOI: 10.1016/j.cell.2019.07.008"The Pancreatic Cancer Microbiome Promotes Oncogenesis by Induction of Innate and Adaptive Immune Suppression"
Cancer Discovery, 2018
DOI: 10.1158/2159-8290.CD-17-1134"Potential role of intratumor bacteria in mediating tumor resistance to the chemotherapeutic drug gemcitabine"
Science, 2017
DOI: 10.1126/science.aah5043"The human tumor microbiome is composed of tumor type-specific intracellular bacteria"
Science, 2020
DOI: 10.1126/science.aay9189"The fungal mycobiome promotes pancreatic oncogenesis via activation of MBL"
Nature, 2019
DOI: 10.1038/s41586-019-1608-2"Identification of unique neoantigen qualities in long-term survivors of pancreatic cancer"
Nature, 2017
DOI: 10.1038/nature24462"A faecal microbiota signature with high specificity for pancreatic cancer"
Gut, 2022
DOI: 10.1136/gutjnl-2021-324755"Oral Bacterial and Fungal Microbiome and Subsequent Risk for Pancreatic Cancer"
JAMA Oncology, 2025
DOI: 10.1001/jamaoncol.2025.3377"The microbiome-derived metabolite TMAO drives immune activation and boosts responses to immune checkpoint blockade in pancreatic cancer"
Science Immunology, 2022
DOI: 10.1126/sciimmunol.abn0704"Gut microbiota reshaping the pancreatic cancer immune microenvironment: new avenues for immunotherapy"
Molecular Cancer, 2025
DOI: 10.1186/s12943-025-02513-5"The tumour microenvironment in pancreatic cancer — new clinical challenges, but more opportunities"
Nature Reviews Clinical Oncology, 2025
DOI: 10.1038/s41571-025-01077-z"Gut OncoMicrobiome Signatures (GOMS) as next-generation biomarkers for cancer immunotherapy"
Nature Reviews Clinical Oncology, 2023
DOI: 10.1038/s41571-023-00785-8"Tumor ecosystem and microbiome features associated with efficacy and resistance to avelumab plus chemoradiotherapy in head and neck cancer"
Nature Cancer, 2026
DOI: 10.1038/s43018-025-01068-0"Intratumoral bacteria are immunosuppressive and promote immunotherapy resistance in head and neck squamous cell carcinoma"
Nature Cancer, 2026
DOI: 10.1038/s43018-025-01067-1